Target tissue type, as well as a patient’s gender, nutritional, and reproductive status, must be considered to manipulate signaling through the RANKL/RANK pathway for therapeutic benefit. In some contexts, activating this pathway can be beneficial and in others inhibiting this pathway is beneficial. RANKL is the ligand, RANK [receptor activator of nuclear factor kappa-B (NF-κB)] is the receptor, and osteoprotegerin (OPG) is a protein that functions as a natural inhibitor of RANKL (1).
One of the best-known functions of the RANKL/RANK pathway is promoting the production of the body’s natural bone-degrading cells called osteoclasts. Consequently, biologic agents that inhibit the activity of RANKL, such as the monoclonal antibody denosumab, are used to prevent osteoporosis and treat cancers or cancer metastases that involve bone degradation, including breast cancer. In those contexts, inhibition of the RANKL/RANK pathway is therapeutically beneficial.
However, this pathway also plays an important role in epithelial cell proliferation and differentiation in several organs, including the breast and thymus. Indeed, RANK is a receptor that is ubiquitously present throughout the body and is particularly abundant in skeletal muscle, thymus, liver, colon, small intestine, and adrenal gland. Whether it is therapeutically beneficial to inhibit this pathway depends on the context.

Because inhibition of the RANKL/RANK pathway reduces proliferation of epithelial progenitor cells in the breast, antagonizing this pathway may be reduce or delay the occurrence of breast cancer (2). However, the changes that occur during pregnancy that enable lactation require RANKL/RANK signaling. Thus, inhibiting this pathway would be detrimental in a pregnant woman or in one seeking to become pregnant (Figure 1).
What about inhibiting this pathway after a woman has given birth? Studies with mice provide some insight. Although mice genetically engineered to lack this pathway cannot lactate (1), lactation occurs normally if this pathway is pharmacologically inhibited after birth of the pups by giving the mothers OPG to block RANKL activity (3). Only when dietary calcium was limited did OPG-mediated inhibition of RANKL/RANK signaling compromise milk production, lead to hypocalcemia (too little calcium in circulation) and cause death of some of the lactating mice. Not only did lactating mice fed a nutritionally complete diet and administered OPG have normal milk production, they also did not exhibit the normal reduction in bone mass that occurs during lactation and the restoration in bone mass that occurs after weaning. Bone mass remained unchanged in the OPG-treated mice if the diet had sufficient calcium. This study indicates that nutritional status, particularly dietary calcium, is critically important for determining the consequences of inhibition of RANKL/RANK signaling during lactation.
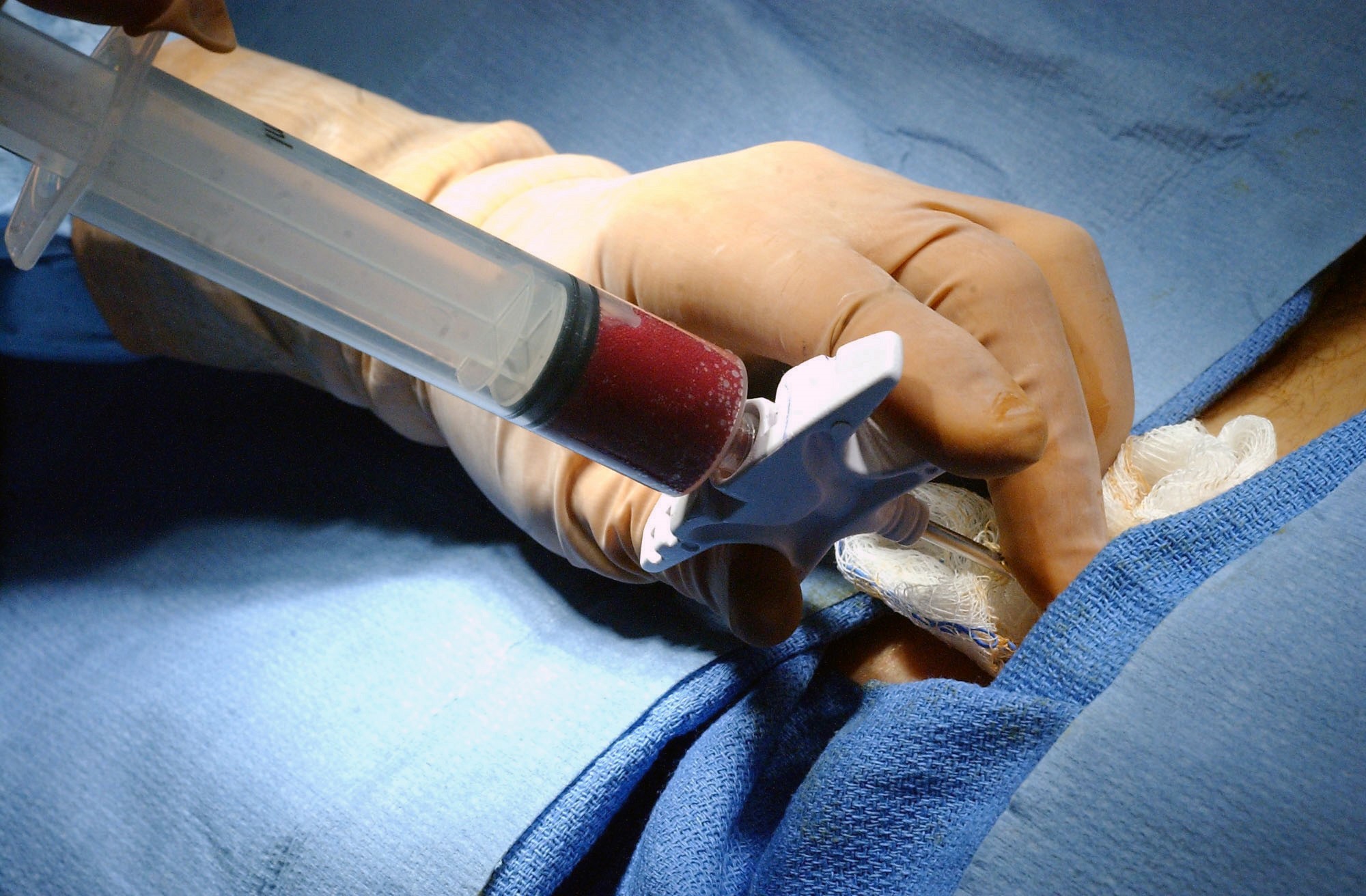
In the thymus, RANKL/RANK signaling is important for the maintenance of the thymic epithelial cells. T cells generated by the bone marrow interact with thymic epithelial cells, including those that present “self” antigens to the T cells to prevent the proliferation of autoreactive T cells and the development of autoimmunity. Patients that require a bone marrow transplant (Figure 2) first have their immune system destroyed by radiation or chemotherapy, both of which not only kill the dividing cells in the bone marrow but also kill the dividing cells in the thymus. The bone marrow transplant does not restore these thymic cells, so they must regenerate. The time required for the regeneration of the thymic cells represents a period of compromised immunity, which can lead to infection, autoimmunity or tumor relapse.
Lopes and colleagues investigated if enhanced RANKL/RANK signaling promoted regeneration of thymic epithelial cells and shortened the period of recovery after bone marrow transplant in mice. Mice receiving total body irradiation increased the abundance of RANKL in two populations of cells in the thymus, CD4+ T cells and lymphoid tissue inducer cells. Administration of an antibody that blocks RANKL function not only prevented regeneration of thymic epithelial cells in the mice receiving total body irradiation, but this treatment also reduced the number of thymic epithelial cells compared with those in the mice that received only the irradiation. In contrast, administration of RANKL-GST (RANKL fused to another protein to enhance its stability) increased the number of thymic epithelial cells, including those that limit autoreactive T cells, compared with the number of these cells in mice only receiving total body irradiation. These initial experiments confirm the importance of RANKL/RANK signaling in thymic regeneration.

Compared with the recovery of young patients, the recovery of the immune system following bone marrow transplant is less efficient and slower in elderly patients (Figure 3). Lopes and colleagues showed that both young and aged mice receiving RANKL-GST treatment after bone marrow transplant exhibited enhanced recovery of all thymic epithelial cell populations and reconstitution of the T cell populations from the donor mouse used for the bone marrow transplant. This study suggests that RANKL therapy or activation of the RANKL/RANK pathway may speed immune system recovery in patients receiving bone marrow transplants and may also be useful in patients with aging related compromised immune function or immune system damage due to radiation exposure.
Together, these studies illustrate how critical context is when deciding whether the activity of a particular signaling pathway should be enhanced or inhibited for therapeutic benefit. The contexts described here include the tissue or organ that is the intended target and the patient’s nutritional status, reproductive status, and gender. Gender and reproductive status are important considerations for using RANKL inhibitors to treat cancer patients with bone-metastasizing cancer. Reproductive status is important when considering the use of denosumab as a possible breast cancer preventative. Inhibition is appropriate if the goal is maintaining bone mass, whereas enhancement of this pathway is appropriate when the goal is restoration of thymic function.
Related Reading
- V. Sigl, L. P. Jones, J. M. Penninger, RANKL/RANK: from bone loss to the prevention of breast cancer. Open Biol.6: 160230 (2016). PubMed
- N. R. Gough, Can denosumab prevent breast cancer? Bioserendipity(10 May 2017). https://www.bioserendipity.com/2017/05/10/denosumab-breast-cancer/
- L. Ardeshirpour, C. Dumitru, P. Dann, J. Sterpka, J. VanHouten, W. Kim, P. Kostenuik, J. Wysolmerski, OPG treatment prevents bone loss during lactation but does not affect milk production or maternal calcium metabolism. Endocrinology 156, 2762-2773 (2015). doi: 10.1210/en.2015-1232 PubMed
- N. Lopes, H. Vachon. J. Marie, M. Irla, Administration of RANKL boosts thymic regeneration upon bone marrow transplantation. EMBO Mol. Med. 9, 835-851 (2017). PubMed
Cite as: N. R. Gough, Therapeutic Applications for Inhibitors and Activators of RANKL/RANK Signaling. BioSerendipity (9 June 2017). https://www.bioserendipity.com/2017/06/09/therapeutic-applications-for-inhibitors-and-activators-of-ranklrank-signaling/