What is a vaccine?
A vaccine may be described as medicine that stimulates an immune response with a “memory.” Many people also consider a vaccine to be a medicine that prevents a disease caused by a pathogen. Indeed, the first vaccines were ones that prevented infectious diseases, such as polio and measles. Some vaccines have been so successful that vaccines against those diseases are not needed anymore. Smallpox, which is caused by variola virus, is an example of a disease eliminated through effective vaccination. Another is polio, which has been eliminated from many countries.
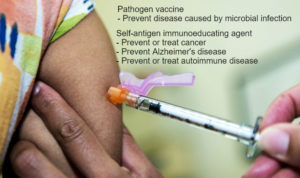
However, the term “vaccine” is also used for therapeutics under investigation for the treatment or prevention of diseases that are not caused by pathogens. Some of the investigations target autoimmune diseases, which are caused by the inappropriate recognition of self molecules in the body. These molecules inappropriately function as “self-antigens” and stimulate an inflammatory immune response. Other studies attempt to use self-antigens to make the immune system recognize abnormal cells or molecules and thus prevent or treat diseases, like cancer and Alzheimer’s disease, caused by these abnormal cells or molecules.
How do vaccines work?
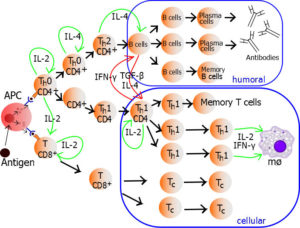
The human immune system has an adaptive part and an innate part. Both parts are important to the response to a vaccine. All vaccines contain molecules that function as antigens, and some vaccines also contain molecules that function as irritants to help the immune system respond to the antigen. Antigens are molecules that stimulate a response from the adaptive part of the immune system and trigger the production of antibodies by B cells and a type of T cells called effector or cytotoxic T cells. Vaccines used to prevent pathogen-caused disease can contain one or more antigens that have been isolated from the pathogen. Alternatively, a vaccine can contain an attenuated (a weakened and less infectious) form of the pathogen. Vaccines can also be made from engineered viruses that carry in their DNA the information to make specific antigens that will trigger immunity and prevent disease.
Some vaccines require multiple exposures (boosters) to produce a sufficiently robust memory response, and some vaccines require ongoing boosters throughout a person’s life to maintain the immunized state. For example, the vaccine against Clostridium tetani, the species of bacteria that causes tetanus (commonly referred to as Lockjaw), requires lifetime boosters. A person with a puncture wound or skin injury from metal will be asked, “Have you had a tetanus shot?” or “When was your last tetanus shot?” The healthcare professional is asking when the injured person was last vaccinated against Clostridium tetani to determine whether the person is still immunized or needs a booster vaccine.
Thus, vaccines are drugs that “teach” the immune system about one or more antigens. Once educated by a vaccine, the immune system can remember the antigen(s) and react rapidly. Indeed, the immune system responds so quickly that the pathogen with the antigen cannot grow quickly enough to cause disease or be contagious to other people.
Can vaccines be used against self-antigens?
The term “vaccine” has also been applied to therapeutic strategies that use self-antigens to teach or re-educate the immune system. These types of vaccines or vaccine-like therapies are under investigation to train the immune system to recognize cancerous or precancerous cells or proteins associated with Alzheimer’s disease, to alter the immune response to prevent type 1 diabetes (a form of autoimmune disease), and to train a form of innate immune cells (dendritic cells) to treat autoimmune arthritis. These rely on antigen-mediated training of the immune system, like vaccines against pathogens. However, using the term vaccine for these can be confusing, because there is no pathogen involved and some strive to reduce an inappropriate immune response rather than promote a beneficial one.
The cancer vaccine concept is even more confusing, because some cancers are caused by infection, such as cervical cancer, which is caused by human papillomaviruses (HPV), and some forms of stomach cancer, which can be caused by the bacterium Helicobacter pylori. For infection-related cancers, the vaccine functions exactly as any vaccine against a pathogen: The vaccine triggers immunity that prevents the pathogen from establishing an infection and causing disease. Without establishing the infection, the virus or bacteria cannot cause cancer. Thus, the HPV vaccine is both a pathogen vaccine and a cancer vaccine.
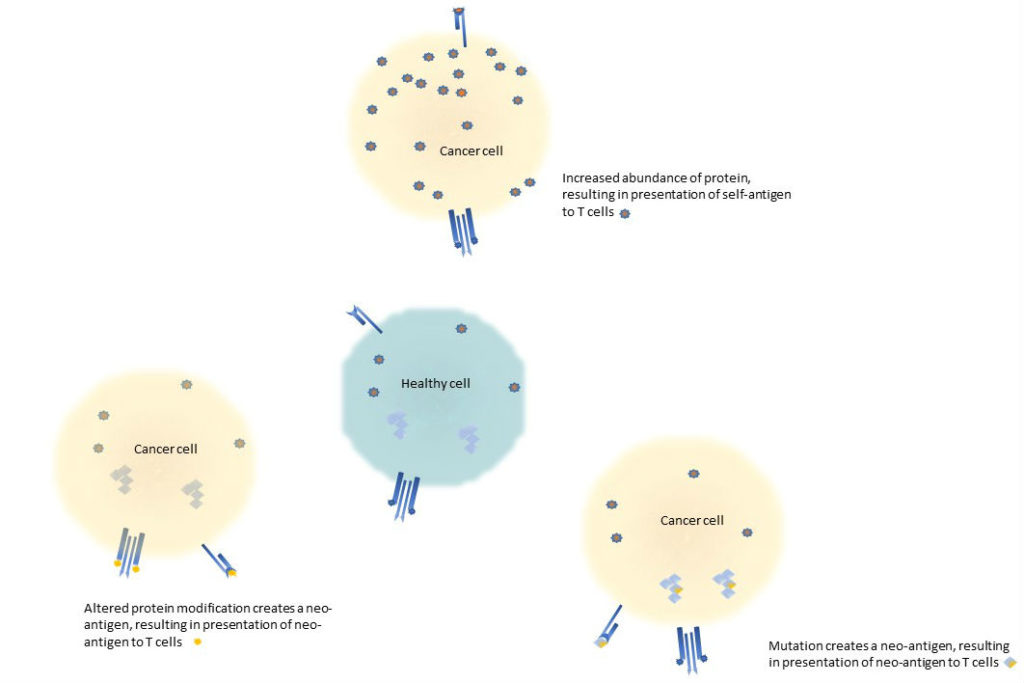
The other types of cancer vaccines use self-antigens (Figure 2). They are intended to prevent cancers with (i) mutations that create proteins with neo-antigens (new antigens), (ii) mutations that cause excessive production of a protein or the appearance of a protein at the cell surface, or (iii) biochemical changes that alter the modifications on proteins or lipids. In theory, any of these changes could make the cancer cells sufficiently different from normal cells that the cancer cells contain antigens that could be recognized and thus the cancer cells destroyed by the immune response. If these cancer-associated self-antigens could be identified and used to create a vaccine, then the vaccine would train the immune system to recognize the cancer cells with the self-antigen used in the vaccine. If the vaccine were given before a person ever developed symptomatic or detectable cancer, then presumably the cancer cells would be eliminated quickly enough by the immune system to prevent disease. Cancer vaccines could also be used therapeutically to help the immune system mount a response to an established cancer. However, any immune evasion strategies used by the cancer would have to be overridden to enable such a therapeutic benefit.
The Alzheimer’s disease vaccines also rely on self-antigens. These self-antigens are present in the protein Aβ42, which is a protein cleavage product associated with Alzheimer’s disease. The goal of the vaccine is to immunize people early enough so that the immune system would prevent the accumulation of this toxic protein product. Assuming the accumulation of Aβ42 causes the cognitive impairment, this vaccine would prevent the disease. The initial studies in animal models showed that the animals mounted an immune response, including antibodies, that recognized human Aβ42. Whether these self-antigen vaccines provide therapeutic benefit in preclinical models of Alzheimer’s disease and whether they are safe for humans remain to be tested.
In autoimmune diseases, such as type 1 diabetes and some forms of arthritis, the immune system mounts an abnormal inflammatory response to normal tissues. The immune system has been trained inappropriately. The vaccine-like strategies used for autoimmune diseases re-train the immune system to reduce the response of the immune system to a self-antigen that it should not recognize. Although these also use self-antigens, the mechanism of disease prevention is different from the cancer and Alzheimer’s disease vaccines. In cancer and Alzheimer’s disease vaccines, the vaccines use self-antigens to stimulate the inflammatory immune response to destroy abnormal cells (cancer) or eliminate abnormal proteins (Alzheimer’s disease). In contrast, the type 1 diabetes and arthritis vaccines use self-antigens to trigger a reduction in the inflammatory immune response to normal tissues or proteins. Thus, the autoimmune disease vaccines have the opposite effect as vaccines against pathogen-associated antigens, the cancer vaccines, and the Alzheimer’s vaccines.
Should vaccines targeting self-antigens have a different name?
Unfortunately, many people are scared by vaccines. Using this term more broadly than for prevention of disease caused by pathogens may add to the confusion surrounding these essential medicines for improving and maintaining world health. Common sources of information, such as Wikipedia and the U. S. Department of Health and Human Services, describe vaccines in terms of preventing infectious disease. Maybe the term vaccine should be restricted to therapeutics that deliver antigens (or DNA encoding antigens) to produce a memory adaptive immune response to prevent disease arising from infection with a pathogen.
It is easy to understand how the idea that we are vaccinating against ourselves (self-antigens) does not make sense to some people. The potential adverse effects from self-antigen vaccines are likely to be different either in type or intensity from those used to prevent infectious disease. Defining the appropriate recipients for these vaccines based on risk-benefit analysis is likely to be different from the process for establishing who should receive infectious disease-preventing vaccines. Thus, it may serve the scientific community and the public well if self-antigen vaccines were given a different name (Figure 3), such as self-antigen immunomodulators, self-antigen immunoeducating agent, or self-antigen immunotherapy. None of those are as short and sexy (or as fraught with preconceptions) as the term vaccine. Maybe a more descriptive name would help the public accept and understand such therapeutics. The idea of being vaccinated against yourself does not sound like a good idea, even when it really could be.
Related Research Articles
Ali, M.A., Liu, Y.-F., Arif, S., Tatovic, D., Shariff, H. Gibson, V.B., Yusuf, N., Baptista, R.,
Eichmann, M., Petrov, N., Heck, S., Yang, J.H.M., Tree, T.I.M., Pujol-Autonell, I., Yeo, L., Baumard, L. R., Stenson, R., Howell, A., Clark, A., Boult, Z., Powrie, J., Adams, L., Wong, F.S., Luzio, S., Dunseath,G., Green, K., O’Keefe, A., Bayly, G.,Thorogood, N., Andrews, R., Leech, N., Joseph, F., Nair, S., Seal, S., Cheung, H., Beam, C., Hills, R., Peakman, M., Dayan, C.M., Metabolic and immune effects of immunotherapy with proinsulin peptide in human new-onset type 1 diabetes. Sci. Transl. Med. 9, eaaf7779 (2017). https://www.ncbi.nlm.nih.gov/pubmed/28794283
Benham, H., Nel, H.J., Law, S.C., Mehdi, A.M., Street, S., Ramnoruth, N., Pahau, H., Lee, B.T., Ng, J., Brunck, M.E.G., Hyde, C., Trouw, L.A., Dudek, N.L., Purcell, A.W., O’Sullivan, B.J., Connolly, J.E., Paul, S.K., Cao, K.-A.L., Thomas, R., Citrullinated Peptide Dendritic Cell Immunotherapy in HLA Risk Genotype–Positive Rheumatoid Arthritis Patients. Sci. Transl. Med. 7, 290ra87-290ra87 (2015). https://www.ncbi.nlm.nih.gov/pubmed/26041704
Lambracht-Washington, D., Fu, M., Frost, P., Rosenberg, R.N., Evaluation of a DNA Aβ42 Vaccine in Adult Rhesus Monkeys (Macaca mulatta): Antibody Kinetics and Immune Profile after Intradermal Immunization with Full-Length DNA Aβ42 Trimer. Alzheimers Res. Ther. 9, 30 (2017). https://www.ncbi.nlm.nih.gov/pubmed/28441965
Lambracht-Washington, D., Fu, M., Wight-Carter, M., Riegel, M., Rosenberg, R.N., 2017b. Evaluation of a DNA Aβ42 Vaccine in Aged NZW Rabbits: Antibody Kinetics and Immune Profile after Intradermal Immunization with Full-Length DNA Aβ42 Trimer. J. Alzheimers Dis. 57, 97–112 (2017). https://www.ncbi.nlm.nih.gov/pubmed/28222511
Mulder, C.K., Dong, Y., Brugghe, H.F., Timmermans, H.A.M., Tilstra, W., Westdijk, J., van Riet, E., van Steeg, H., Hoogerhout, P., Eisel, U.L.M., 2016. Immunization with Small Amyloid-β-derived Cyclopeptide Conjugates Diminishes Amyloid-β-Induced Neurodegeneration in Mice. J. Alzheimers Dis. 52, 1111–1123 (2016). https://www.ncbi.nlm.nih.gov/pubmed/27060957
Pang, Z., Higuchi, M., Koriyama, H., Yoshida, S., Kurinami, H., Shimamura, M., Takami, Y., Rakugi, H., Morishita, R., Nakagami, H., Evaluating the Potential of the GFAP-KLH Immune-Tolerizing Vaccine for Type 1 Diabetes in Mice. FEBS Lett. 591, 129–136 (2017). https://www.ncbi.nlm.nih.gov/pubmed/27926781
Related News
Research spotlight– A vaccine for Type 1 diabetes. Diabetes UK (accessed 8.1.17) https://www.diabetes.org.uk/Research/Research-round-up/Research-spotlight/Research-spotlight-a-vaccine-for-Type-1-diabetes/ .
K. Templeman, Rheumatoid arthritis “vaccine” passes big test. Futurity (2015). [Accessed 1 August 2017]
Related Reference Websites
Vaccines.gov. U. S. Department of Health & Human Services (accessed 1 August 2017) https://www.vaccines.gov/basics/index.html
Vaccine. Wikipedia (accessed 1 August 2017) https://en.wikipedia.org/wiki/Vaccine
Update: A relevant study by Ali et al. was added to the Related Research Articles section on 9 August 2017.
Cite as: N. R. Gough, Can you be vaccinated against yourself? BioSerendipity (3 August 2017). https://www.bioserendipity.com/can-you-be-vaccinated-against-yourself/