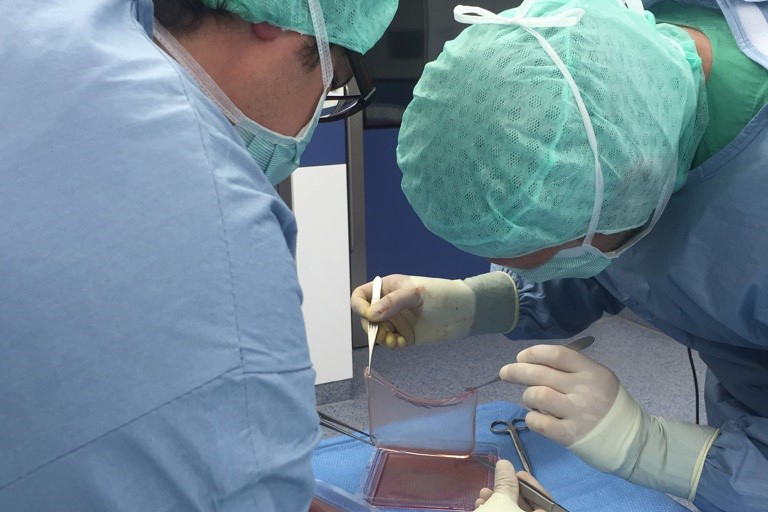
Stem cells hold great promise for medical intervention. However, it has been difficult to leverage these cells effectively. In the study by Hirsch and colleagues, a collaboration between doctors and researchers saved the life of a child with a skin disorder called junctional epidermolysis bullosa (JEB). JEB is a genetic disease caused by mutations in the gene LAMB3 encoding the protein laminin-322. Laminin-322 attaches the epithelial cells to the underlying tissue called the basement membrane. Without this protein, the skin injures very easily and cannot properly repair.
Like blood cells, skin cells do not last an entire lifetime. They die and are constantly renewed by specialized stem cells throughout a person’s life. The doctors sent a skin biopsy from the patient to the researchers who isolated stem cells from the skin sample. Using molecular biology, the researchers engineered a virus to contain the nonmutated gene and infected the stem cells in culture with this virus. The stem cells integrated the nonmutant gene into their DNA and grew in culture on special support structures into sheets of epidermis (Figure 1).
When these virally-modified sheets of epidermal cells were grafted onto the patient, they contained some stem cells as well as the differentiated epidermal cells. All of the cells had the gene that made nonmutated laminin-322. These engineered cells fixed the underlying defect. The transplanted epidermal sheets containing the stem cells ultimately formed injury-resistant normal skin. Additionally, the transplanted stem cells retained the properties of stem cells: They formed new stem cells (a property called self-renewal) and they differentiated into normal skin and may even form the cells that generate hair. [Note added 2 February 2018: The authors do not have definitive evidence that the hair follicles were formed by the transgenic, transplanted stem cells.] Two years after receiving the transplanted skin cells, the child has recovered fully. Hopefully, the engineered skin stem cells will continue to function for the rest of his life.
This study illustrates an example of patient-derived, cell-based therapy achieved through (i) isolation of tissue-specific stem cells, (ii) viral-mediated gene therapy, and (iii) ex vivo growth of differentiated cells using specialized scaffolds in culture. It shows the power of combining different fields of science— molecular biology, synthetic biology, cell biology, genetics, and materials science—to produce patient-specific, life-saving, personalized medicine.
Highlighted Research
T. Hirsch, T. Rothoeft, N. Teig, J. W. Bauer, G. Pellegrini, L. D. Rosa, D. Scaglione, J. Reichelt, A. Klausegger, D. Kneisz, O. Romano, A. S. Seconetti, R. Contin, E. Enzo, I. Jurman, S. Carulli, F. Jacobsen, T. Luecke, M. Lehnhardt, M. Fischer, M. Kueckelhaus, D. Quaglino, M. Morgante, S. Bicciato, S. Bondanza, M. D. Luca, Regeneration of the entire human epidermis using transgenic stem cells, Nature 551, 327 (2017). PubMed
News and Commentary
H. Devlin, Scientists grow replacement skin for boy suffering devastating genetic disorder. The Guardian (8 November 2017). https://www.theguardian.com/science/2017/nov/08/scientists-grow-replacement-skin-for-boy-suffering-devastating-genetic-disorder
Boy is given new skin thanks to gene therapy. Ruhr-University Bochum (8 November 2017) http://news.rub.de/presseinformationen/wissenschaft/2017-11-08-weltweit-einzigartig-junge-erhaelt-dank-gen-therapie-neue-haut
Genes and Proteins
LAMB3, UniProt (accessed 5 December 2017) http://www.uniprot.org/uniprot/Q13751
Cite as: N. R. Gough, Virally Modified Cells Regenerate Normal Skin. BioSerendipity (5 December 2017). https://www.bioserendipity.com/virally-modified-cells-regenerate-normal-skin/