Lyme disease is caused by bacteria (Borrelia burgdorferi, Borrelia afzelii, and Borrelia garinii) that are delivered by a bite from an infected tick (Figure 1). The Centers for Disease Control (1) recommend a preventative (prophylactic) single dose of the antibiotic doxycycline for adults bitten by a mosquito with a high probability of carrying the Lyme-causing bacteria. No such prophylactic option is yet recommended for children under 8 years old, and there is no appropriate antibiotic that can be given to pregnant women. This short antibiotic course of prophylaxis is not accepted by all doctors (2). Some favor the full course of treatment. Fortunately, new strategies for providing protection are under investigation.
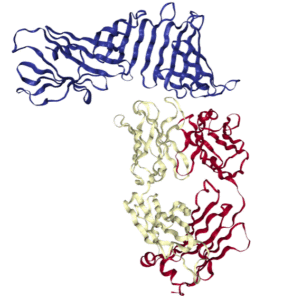
A vaccine would be the most common option for preventing an infectious disease. However, the only Lyme vaccine that made it to FDA approval was subsequently withdrawn from the market, because some people receiving the vaccine complained of arthritis-like symptoms (3). Unfortunately, the vaccine was withdrawn by the manufacturer before conclusive testing could be performed to determine the true risk of adverse effects. Research revealed that some people may be genetically predisposed to develop an autoimmune reaction triggered by the bacterial protein (OspA, Figure 2) used in the vaccine. In these people, the antibodies triggered by the vaccine could also recognize self-proteins, thereby causing the vaccine-induced arthritis.
Another vaccine that uses the OspA proteins from the various strains of the bacteria that cause Lyme disease is in clinical trials in the US and Europe (4). This vaccine may have some advantages over the first one that was withdrawn. Rather than using the complete OspA protein from a single bacterial strain that causes Lyme disease, the new vaccine includes OspA fragments from multiple bacterial variants (5). Thus, this vaccine should be effective against more than on type of Lyme disease-causing bacteria, may not include the part of the protein that can trigger autoimmune responses, and should be useful in more places.
The first OspA-based vaccine that was withdrawn only provided protection to only ~80% of the people receiving vaccine and required multiple boosters. Some people receiving the vaccine may have had a false sense of security, because it was not known who represented the 20% that were not protected. Hopefully, any new vaccines will be thoroughly examined in enough patients to determine (i) the safe population in which they can be administered, which may require testing for specific properties of the immune system to avoid generating autoimmune responses, and (ii) if the new vaccine will protect a greater percentage of recipients than the 80% coverage provided by the first one.

Another strategy for prevention relies on identifying human antibodies that recognize OspA and kill the bacteria but do not also recognize normal proteins in humans. These antibodies would then be injected into at-risk people before the start of the tick season in areas where Lyme disease is common. Wang and colleagues (6) used genetically engineered mice to generate human antibodies against OspA. One of the antibodies killed the 3 common species of Lyme disease-causing bacteria in culture. Experiments with mice showed that a single injection of this antibody completely protected mice from infection by ticks carrying Borrelia burgdorferi, the bacteria that causes Lyme disease in the US. The next steps are discussions with the FDA regarding a Phase I clinical trial (7). Unlike a vaccine, which generates multiple antibodies and a long-term memory in the immune system and thus lasts years or for a person’s lifetime, this single antibody treatment would be a “biologic” agent that at-risk people would receive annually (Figure 3). The idea is that when the tick bites a person who had received the antibody injection, the tick would ingest the antibody and the bacteria would be killed in the tick, thereby preventing transmission of the bacteria to the person (8). The hope is that the potential for adverse effects would be minimized by injecting a single optimized antibody that prevents infection rather than waiting for an infection and the immune response that follows.
This idea of injecting an antibody as a drug is not a new one. Indeed, many anticancer biologic therapies and biologic treatments for autoimmune diseases, such as arthritis and Crohns disease, are antibodies. What is new, to me at least, is the idea of injecting people with an antibody to eliminate an infection in ticks so that the ticks cannot transmit the bacteria to the person. Taking a lesson from the cancer therapy field and applying it to the infectious disease field leads me to speculate whether synthetic biology may have a role here as well. Can a person’s immune cells could be engineered using synthetic biology to generate the antibody against the pathogen and thus provide a long-lasting response?
References
- Tickborne Diseases of the United States: A Reference Manual for Health Care Providers. 4th Edition (2017) Center for Disease Control, U.S Department of Health and Human Services. https://www.cdc.gov/lyme/resources/TickborneDiseases.pdf
- B. Stringfellow, Visiting physician sheds new light on Lyme disease. MV Times (13 July 2016). http://www.mvtimes.com/2016/07/13/visiting-physician-sheds-new-light-lyme-disease/
- L. E. Nigrovic, K. M. Thompson, The Lyme Vaccine: A Cautionary Tale. Epidemiol. Infect. 135, 1-8 (2007). PubMed
- P. La Vigne, B. L. Fisher, FDA Gives Green Light to Test Lyme Disease Vaccine in Humans. The Vaccine Reaction (26 January 2017). http://www.thevaccinereaction.org/2017/01/fda-gives-green-light-to-test-lyme-disease-vaccine-on-humans/
- P. Comstedt, M. Hanner, W. Schüler, A. Meinke, U. Lundberg, Design and Development of a Novel Vaccine for Protection against Lyme Borreliosis. PLoS ONE 9, e113294 (2014). PubMed
- Y. Wang, A. Kern, N. K. Boatright, Z. A. Schiller, A. Sadowski, M. Ejemel, C. A. Souders, K. A. Reimann, L. Hu, W. D. Thomas, Jr, M. S. Klempner, Pre-exposure Prophylaxis with OspA-Specific Human Monoclonal Antibodies Protects Mice Against Tick Transmission of Lyme Disease Spirochetes. J. Infect. Dis. 214, 205-211 (2016). PubMed
- M. Szaniszlo, Lyme drug eyed for human trials. Boston Herald (21 July 2017) http://www.bostonherald.com/news/local_coverage/2017/07/lyme_drug_eyed_for_human_trials
- J. L. Mattern, Scientists are developing a new shot that protects against Lyme disease. WBALTV11 (21 July 2017) http://www.wbaltv.com/article/new-lyme-disease-vaccine/10340506
Clinical Trials
Phase 1/2 Lyme Vaccine Study of Multivalent Recombinant OspA Lyme Borreliosis Vaccine. https://clinicaltrials.gov/ct2/show/NCT01504347
Study Assessing the Safety, Immunogenicity and Dose Response of VLA15, A New Vaccine Candidate Against Lyme Borreliosis. https://clinicaltrials.gov/ct2/show/NCT03010228
Drugs
Cite as: N. R. Gough, New Hope for Lyme Disease Prevention. BioSerendipity (27 July 2017) https://www.bioserendipity.com/2017/07/27/new-hope-for-lyme-disease-prevention/